Bionic eyes: no longer science fiction
Over the past decade, there has been an explosion of interest in ‘bionic eyes’, with companies in different parts of the world using different approaches and technologies to develop prostheses to give blind and visually-impaired people a sense of ‘sight’ or, better still, some useable vision.
The leading contenders in the race to find the holy grail of bionic vision are California-based company Second Sight, Australia’s Bionic Vision Technologies and France’s Pixium Vision.
Second Sight’s Argus II
Second Sight has led the pack with its Argus II epiretinal implant, the first technology of its kind to receive regulatory approval for commercial use in Europe (2011) and the USA (2013). Argus II users wear a pair of spectacles with a small camera embedded, so the visual input of the camera can be translated into a series of electrical pulses that the epiretinal implant delivers to the neural circuits of the eye.


UK-based Ray Flynn, wearing his Argus II after it was implanted in 2015. Credit: Second Sight
The Argus II Retinal Prosthesis System allows users to differentiate light from dark backgrounds and see movement, with some gaining ‘finger counting’ acuity. Three visual function tests were investigated: square location (SL), direction of motion and grating visual acuity (GVA). Forty-seven patients were studied for 12 months or longer post-implant. Patient accuracy (averaged across the group) on the SL test and also the GVA test appeared better when the implant was on, but this was not so with the direction of motion test. Serious adverse events were experienced by 26% of the patient group.
A 2016 paper investigating improvements in quality of life (QoL) in Argus II patients, reported that in the three significant QoL dimensions of getting injured, coping with life demands and fulfilling their life’s role, significant improvements occurred after Argus II implantation. Furthermore, the benefits did not deteriorate at any point during the 36 months of follow-up, suggesting a long-term durable improvement.
The Orion
Although there are now more than 300 Argus II users around the world, Second Sight has effectively mothballed this technology to concentrate on its newer technology, the Orion, a visual cortical prosthesis system that bypasses the damaged eye or optic nerve pathways entirely and interfaces with the visual cortex. Whereas the Argus II was specifically designed to help retinitis pigmentosa patients, because Orion bypasses the optic nerve, it can be used to help any patient with an undamaged visual cortex, thus making it more commercially viable.

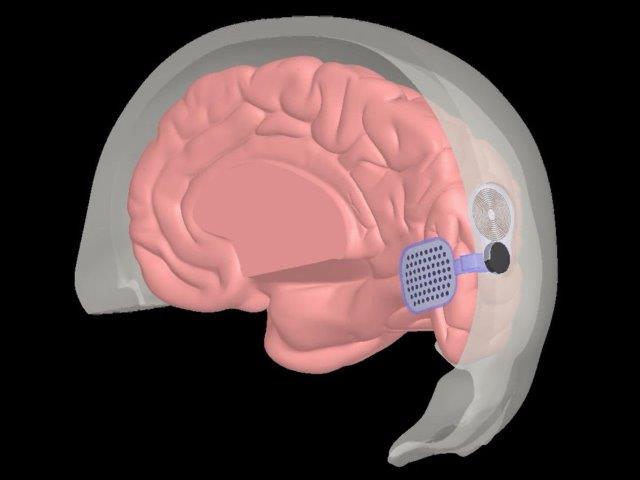
The Orion system
Like the Argus II, however, Orion patients wear a miniature camera mounted on a pair of glasses, an antenna and a video-processing unit (VPU) to convert what the camera sees into electrical impulses. These are then transmitted wirelessly to an electrode array implanted directly on the surface of the primary visual cortex, allowing the wearer to create a perceived image. The Orion device also includes a belt with a button to amplify dark objects in the sun or light objects in the dark. Six subjects have been implanted so far, with average post-implant time being 12 months. Early feasibility studies have shown positive results, but there is also a higher risk of adverse effects, such as serious infection and seizures.
BVT’s Gen2
In January this year, after more than a decade of research, Bionic Vision Technologies (BVT) released interim results for its Gen2 pilot study. BVT is a collaboration between Australian medical science and technology research organisations, including the Centre for Eye Research Australia (CERA), the Bionics Institute, CSIRO’s Data61, the University of Melbourne and the Australian National University.

BVT's bionic eye system
It’s Gen2 bionic eye system consists of a wearable device and a visual implant, similar in concept and design to that used by cochlear implants for hearing. The BVT Gen2 patient’s live video feed, captured through a small video camera mounted on their glasses, is processed and transmitted via a microchip to an electrode array implanted in the patient’s suprachoroidal space between the choroid and sclera. Research has shown this appears to be a safer option than subretinal or epiretinal implantation and avoids damage to an already compromised retina. The electrodes stimulate remaining cells in the retina to generate spots of light known as phosphenes that give the patient a sense of vision by allowing them to experience ‘seeing’ light without light actually entering the eye. What a person ‘sees’ is a series of light flashes, which the patient’s brain is then taught to interpret to ‘see’ their environment.
Another advantage of placing the implant behind the retina is patients can still participate in other remedies being developed, such as gene or stem cell therapies. The stability and lack of serious adverse events also bodes well for future commercialisation, though a timeframe for this is uncertain at this stage.
Since 2012, a total of seven patients have received the implant at the Royal Victorian Eye and Ear Hospital (RVEEH). But surgery is just the first step, said BVT’s lead surgeon Associate Professor Penny Allen, head of RVEEH’s vitreoretinal unit. “These patients have had no useful visual information for more than 15 years, so they need to learn to interpret the flashes of light. The patients all work hard – very hard.”

BVT lead surgeon, RVEEH's Dr Penny Allen
BVT’s Gen2 pilot study focused on retinitis pigmentosa (RP) volunteers. Participants needed a healthy optic nerve and some residual photoreceptor cells in the retina. There’s currently no intention to use BVT’s bionic eye technology for macular degeneration (MD) sufferers as it’s primarily designed for navigation, which is not the issue for MD patients, said A/Prof Allen.
After 44 weeks of active use of the implant, the four RP patients in the pilot study demonstrated improved performance in all functional vision tests. Each participant was unilaterally implanted with the Gen2 prosthesis in the eye with the least remaining vision. Mobility testing was initiated after a two-month post-surgical healing period followed by 16 weeks of vision rehabilitation training. Participants were asked to complete a series of tests at three-month intervals with the device turned on and off. Initial results show participants could identify 74.3% of obstacles in their pathway when the device was turned on, compared to only up to 4% reliably when the device was turned off. Considerable improvement was also recorded for the location task, which relied on study participants identifying and touching an object similar to the shape of a window on a wall. Subjects were able to locate and touch the window 70.3% of the time with the device on compared to only up to 24.4% when the device was off. The average touching distance from the window was also improved from 78cm to 14cm indicating greater accuracy.
“The data from this trial demonstrates that the longer patients used the system, the more proficient they become at locating objects, recognising doorways and avoiding obstacles – all of which contributes to a greater sense of mobility and independence in the day to day lives of people who are blind,” said A/Prof Allen. “The device also gives patients a better sense of social connection, something they have missed since the loss of their sight.”
This patient group is still undergoing tests, while BVT has moved on to developing its Gen3 bionic eye system. This will incorporate new algorithms, which will automatically adjust to environmental lighting conditions, while the external device will be smaller, lighter and look more like traditional spectacles to enhance patient comfort and social interaction, said the company.
Pixium Vision
Based in France, Pixium Vision is working with a number of different researchers from a range of different organisations across the world, including Stanford University in California, the Vision Institute in Paris, Moorfields Eye Hospital in London, the Institute of Ocular Microsurgery in Barcelona, the University Hospital in Bonn and UPMC in Pittsburgh, Philadelphia. Its goal is to develop subretinal implants for MD and glaucoma patients as well as those suffering from RP, and it has also recently reported some successful preliminary results for its Prima bionic eye system.

Pixium Vision's Prima system
Pixium’s Prima-FS is a wireless prosthesis in which photovoltaic pixels convert projected light patterns into a local electric current. It is 2mm in width, corresponding to approximately 7° of the visual angle in a human eye. Images captured by the camera are processed and projected onto the retina from video glasses using near-infrared light to avoid the photophobic and phototoxic effects of bright light. The wireless nature of the Prima-FS implant greatly simplifies the surgical procedure compared with the wired-retinal prosthesis, said Pixium Vision.
In its most recent study, none of the patients enrolled had any remaining central visual activity. All underwent visual rehabilitation post-surgery and at 12 months most could identify patterns, numbers or letters, with speed and accuracy improving continuously during the rehabilitation phase. “Central prosthetic visual acuity measured (with Landolt-C) to date is the best among those published from current visual prosthetic technologies,” said the company. There were no device-related serious adverse events.
Other ‘bionic eye’ breakthroughs
In this burgeoning ‘bionic eye’ field, another breakthrough was reported last year by Swiss scientists from the École Polytechnique Fédérale de Lausanne (EPFL) who have developed a new wireless implant made of a highly flexible material containing photovoltaic pixels. Like conventional implants, EPFL’s implant is composed of an array of pixels, glasses and a camera, but no wires. It also has a larger surface area designed to widen the visual field and improve image quality, said EPFL researchers.
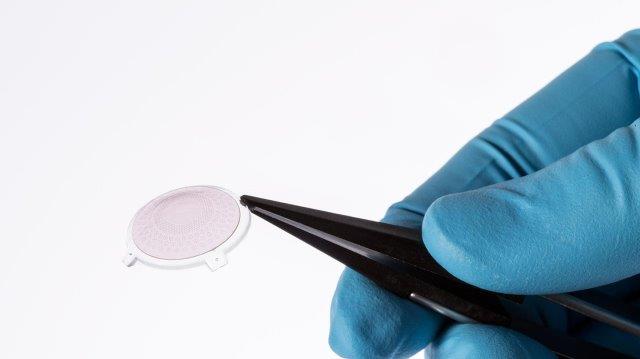
EPFL's highly flexible, wireless retinal implant
A University of Minnesota team of researchers also created a flurry of excitement late last year when they 3D printed an array of light receptors on a hemispherical surface, marking what they described as a significant step in the battle to create the best ‘bionic eye’. Published in Advanced Materials, this US study showed electronics could be printed on a curved surface. The semiconducting polymer materials were then used to print photodiodes, which convert light into electricity. The next step is to create a prototype with more light receptors that are even more efficient and find a way to print on a soft hemispherical material that can be implanted into a real eye, said co-author Associate Professor Michael McAlpine, from Minnesota University’s department of mechanical engineering.
Closer to home, Monash Vision Group, a Melbourne-based collaboration led by Monash University, is gearing up for human trials of its Gennaris bionic vision system, which is also designed to bypass any optic nerve damage and target the brain’s visual cortex directly. “Our design creates a visual pattern from combinations of up to 172 spots of light (phosphenes) which provides information for the individual to navigate indoor and outdoor environments, and recognise the presence of people and objects around them,” said Professor Arthur Lowery, from the Department of Electrical and Computer Systems Engineering.
Monash University's Gennaris system
Meanwhile in Asia, an international team led by scientists at the Hong Kong University of Science and Technology (HKUST) were definitely thinking cyborgs when they released details about their new 3D artificial eye in the middle of this year. Claiming its better than existing bionic eyes and may even exceed human eyes, HKUST’s electrochemical eye (EC-Eye) mimics the human eye’s structure, is sensitive to light and has a faster reaction time than a real eyeball, said research team leader Professor Zhiyong Fan. The EC-Eye has a 3D artificial retina made from an array of nanowire light sensors, which mimic the photoreceptors in human retinas. When these are connected to a bundle of liquid-metal wires, serving as nerves, behind the man-made hemispherical retina, this artificial ‘eye’ successfully replicated the visual signal transmission to reflect what it ‘sees’ on a computer screen.

An artist's impression of HKUST's EC-Eye
“Watching sci-fi series such as Star Trek and I, Robot, I thought about making a ‘super-human eye’ to be used both in humanoid robots and for the visually challenged. At that, my students thought it was yet another crazy idea of the professor,” said Prof Fan. “The resulting biomimetic eye prototype… has 30 times more sensors on the artificial retina than the real human eye. This super-human eye technology, with high imaging resolution, will be ready for integration into medical robots to take care of patients. It will even cater to the visually impaired when we find suitable bio-compatible materials.”
Biomimicry vision
While restoring vision now seems tantalizingly within the realms of possibility, the truth is that instead of focusing on ‘natural’ vision, researchers are concentrating more on how to create practical or useful artificial vision for those who’ve lost their sight. This requires extensive collaboration between neuroscience, computer science, device manufacturers, engineers, software developers and cognitive psychology, so that the multitude of developments in sensors, surgery, wireless technology, data transmission and software, often made in isolation, can be harnessed together, leading to the significant developments of the past two years outlined above.
Though approaches differ and some devices may suit different types of sight-loss better, and there’s always the question of who pays, one thing is clear, bionic eyes are no longer science fiction.
Naomi Meltzer has worked in optometry for more than 30 years. She runs an independent optometry practice specialising in low vision consultancy in Auckland and is a regular contributor to NZ Optics.
Includes additional reporting by Heather Douglas and Lesley Springall