DED and immune-mediated diseases
The most severe forms of chronic dry eye disease (DED) are often caused by underlying immune-mediated diseases. These can be visually debilitating in some cases and treatment may be challenging. Dry eye disease may result directly or indirectly from these conditions, some of which are summarised below. In general, these conditions often require treatment with systemic and/or topical anti-inflammatory medications to reduce the severity of dry eye, particularly in the acute phases of disease.
Sjögren’s syndrome
Sjögren’s syndrome (SS) is classified using a number of diagnostic criteria that include symptoms, signs, histopathologic features and autoantibodies. Clinically, SS can be divided into two subsets: primary SS includes those without a defined systemic immune dysfunction or connective tissue disease, while secondary SS occurs in individuals with a connective tissue disease, most commonly rheumatoid arthritis or another auto-immune disease, such as lupus or scleroderma.
Mechanism of dry eye - Inflammatory infiltration and destruction of the lacrimal glands leads to aqueous tear deficiency with associated ocular surface findings, including punctate epitheliopathy and even filamentary keratitis in severe cases (Fig 1). Similar inflammatory changes may occur in the salivary glands resulting in dry mouth and periodontal disease, although other mucosae (vaginal, gastric, respiratory) may also be affected. Viral infections, including Epstein Barr virus, hepatitis C and HIV, have been associated with Sjögren-like syndromes as well¹.
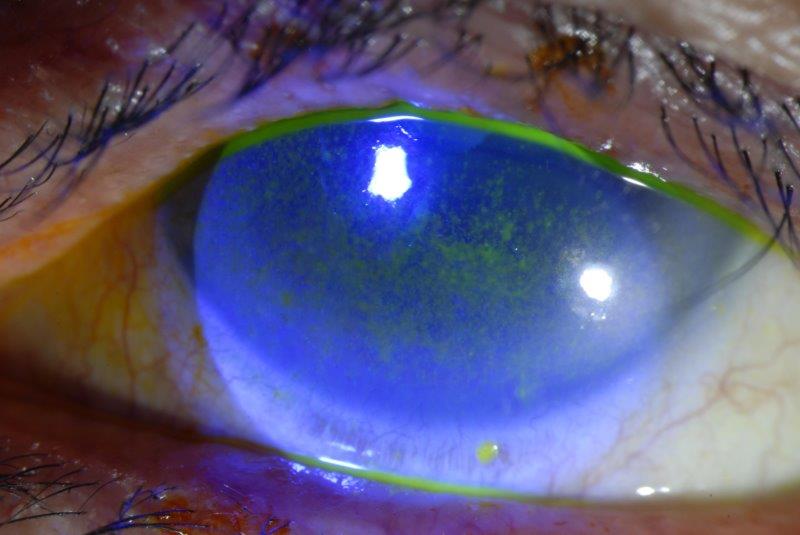
Fig 1. Diffuse punctate corneal fluorescein staining and limbal filament in a patient with Sjögren's syndrome
Treatment considerations - Standard DED treatments can be employed but more advanced treatments, such as punctal occlusion or serum tears, may be required. In patients with active systemic autoimmune inflammation, allogeneic serum tears (from related or unrelated donors) may be preferred due to a theoretical concern of increasing ocular surface inflammation if using autologous serum (from the patient)². Given the underlying immune-mediated process, anti-inflammatory treatment, such as chronic topical cyclosporine or topical corticosteroids in pulsed doses, may be considered or be necessary.
Graft-versus-host disease
Graft-versus-host disease (GVHD) is a complication following bone marrow transplantation, most commonly performed for haematopoietic malignancies. GVHD results from the grafted cells attacking the recipient and may affect multiple tissues, including the eyes, and it can be acute or chronic.
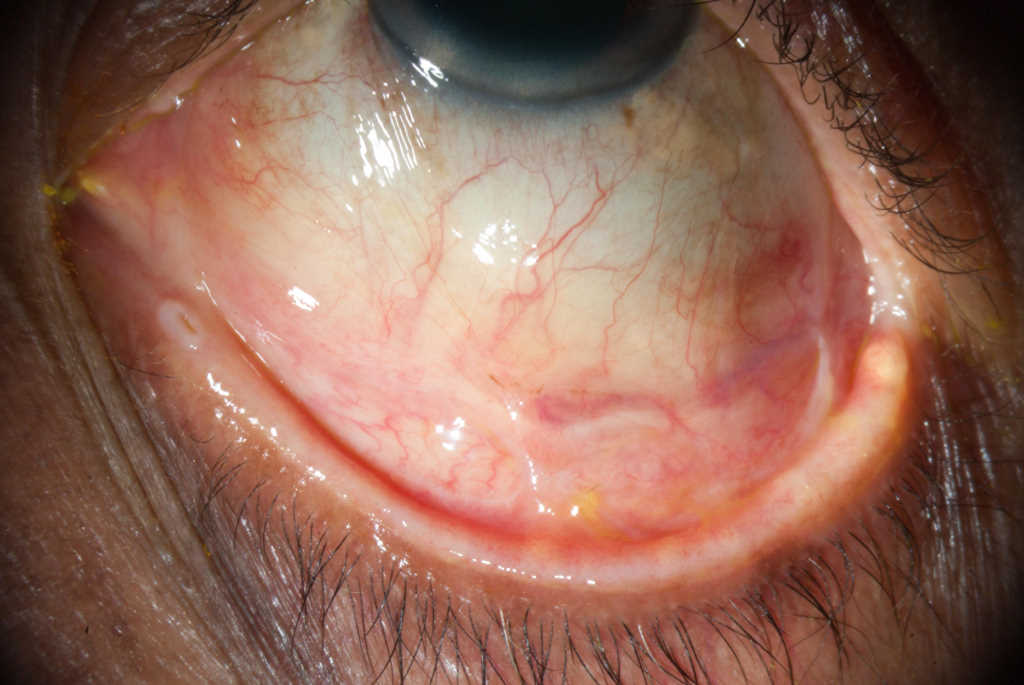
Mechanism of dry eye - Ocular surface damage can result from conjunctival inflammation and lacrimal gland infiltration by lymphocytes. Most commonly, inflammation causes ocular surface dryness due to aqueous tear deficiency, although more severe cases can result in subepithelial fibrosis of the conjunctiva (Fig 2), cicatricial lagophthalmos and even limbal stem cell deficiency and secondary corneal scarring.
Treatment - These individuals frequently have non-ocular GVHD for which they receive potent systemic immunosuppression treatment. In addition, chronic topical anti-inflammatory treatment with topical cyclosporine and/or corticosteroids may be required. Amniotic membrane transplantation can be considered for severe cases.
Thyroid Eye Disease
Thyroid eye disease (TED) results from immune-mediated inflammation of the orbit and develops in a large proportion of individuals with Graves’ disease.
Mechanism of dry eye - Most patients with TED have dry eye disease due to various mechanisms. Evaporative dry eye and corneal exposure may result from the combination of proptosis and lid retraction and subsequent incomplete blinking and nocturnal lagophthalmos. In addition, antibody-induced inflammation and infiltration may lead to lacrimal gland enlargement and abnormalities in the composition of tears³.
Treatment considerations - Ocular lubrication with artificial tears and ointments are the mainstay of treatment. Patients with severe proptosis may require orbital decompression for diplopia, which can also benefit the DED by restoring lid function. Systemic immunosuppression with corticosteroids or other medication may be required for severe TED with active inflammation.
Coeliac Disease
Coeliac disease involves an immune response to dietary gluten that frequently manifests as diarrhoea and weight loss.
Mechanism of dry eye - Malabsorption of nutrients may lead to vitamin A deficiency xerosis due to associated loss of mucus production by the goblet cells, and mild vitamin A deficiency can result in ocular surface dryness. More advanced vitamin A deficiency can lead to Bitot’s spots, or even corneal ulceration (keratomalacia) although deficiency this severe would rarely be due to coeliac disease. Nyctalopia, or night blindness, may be another symptom of hypovitaminosis A. Other non-immune causes of vitamin A deficiency include dietary insufficiency and bariatric surgery leading to malabsorption.
Treatment considerations - Treatment involves systemic replacement of any vitamin A deficiency by a physician. Topical vitamin A ointment can also be administered as an adjunctive treatment.
Immune-mediated disorders of skin and mucous membranes
Oculocutaneous immune-mediated diseases include cicatricial pemphigoid, Stevens-Johnson syndrome, toxic epidermal necrolysis, GVHD, atopic blepharokeratoconjunctivitis and rosacea, among others. These conditions can cause inflammation that leads to destruction of conjunctival goblet cells and, in some cases, obstruction of lacrimal gland ductules. The subsequent aqueous and mucous tear deficiency may lead to keratinisation of the ocular surface as well as corneal vascularisation, scarring and ulceration.
Treatment considerations - The majority of these conditions require systemic immunosuppression to control the inflammation and this is usually prescribed by an immunologist. Topical anti-inflammatory treatment is also frequently necessary and amniotic membrane transplantation may be beneficial. Tacrolimus ointment applied to the eyelids can be a useful alternative to corticosteroids for patients with blepharitis due to atopy or rosacea.
References
1. Ramos-Casals M, Brito-Zerón P, Font J. Lessons from diseases mimicking Sjögren's syndrome. Clin Rev Allergy Immunol 2007;32(3):275-283.
2. Chiang CC, Lin JM, Chen WL, Tsai YY. Allogeneic serum eye drops for the treatment of severe dry eye in patients with chronic graft-versus-host disease. Cornea 2007;26(7):861-863.
3. Khalil HA, de Keizer RJ, Kijlstra A. Analysis of tear proteins in Graves' ophthalmopathy by high performance liquid chromatography. Am J Ophthalmol 1988;106(2):186-190.

Dr Jay Meyer is a subspecialist in cornea/external diseases and glaucoma. He is a consultant ophthalmologist at Eye Institute and the Auckland District Health Board, and a senior lecturer at the University of Auckland.