CASE STUDY: The fun comes undone
A healthy 40-year-old male presented with a one-week history of blurred central vision in his right eye. He had no medical history of note. His left eye was mildly amblyopic. Visual acuity at presentation was counting fingers in the right eye and 6/12 in the left eye. Anterior segments were normal and occasional vitreous cells were noted in the right eye.
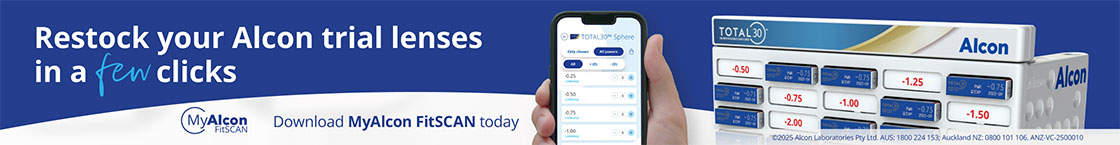
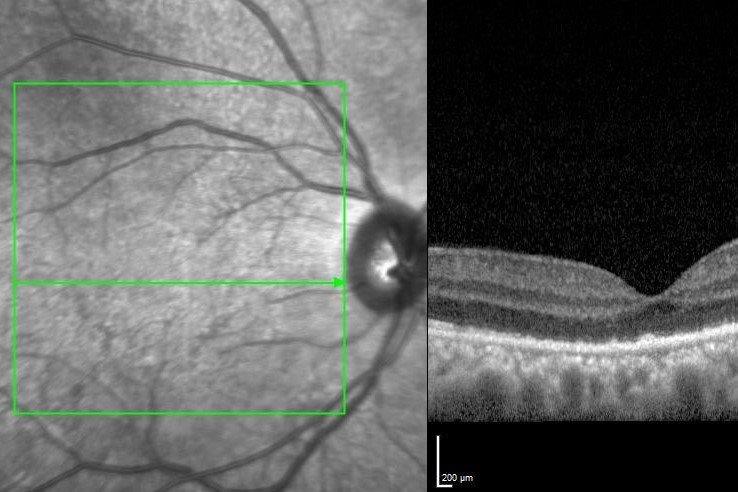
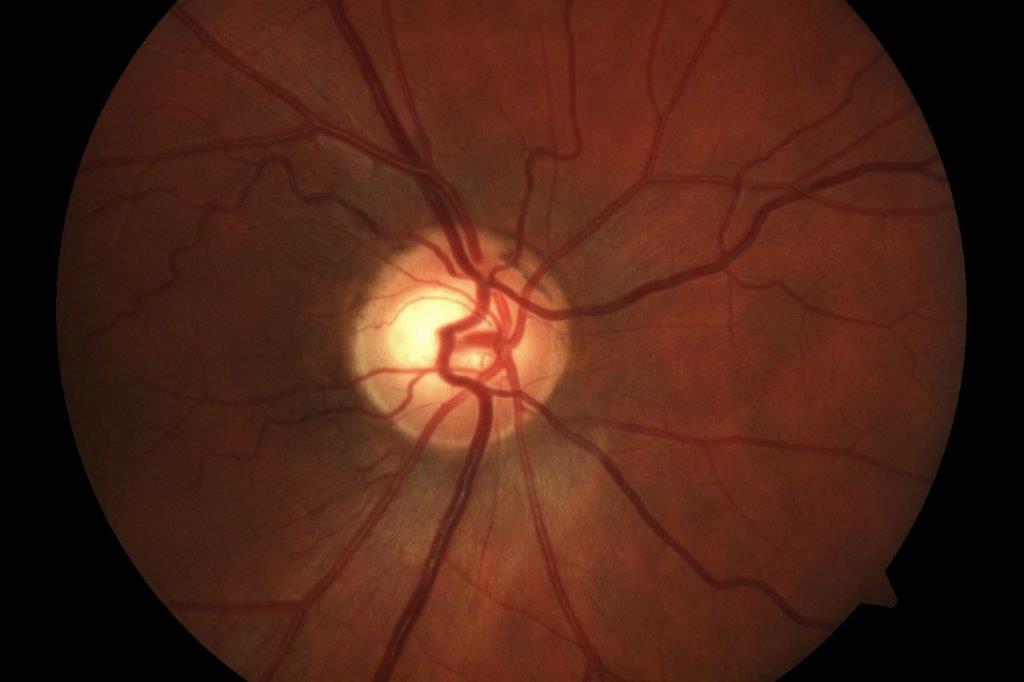
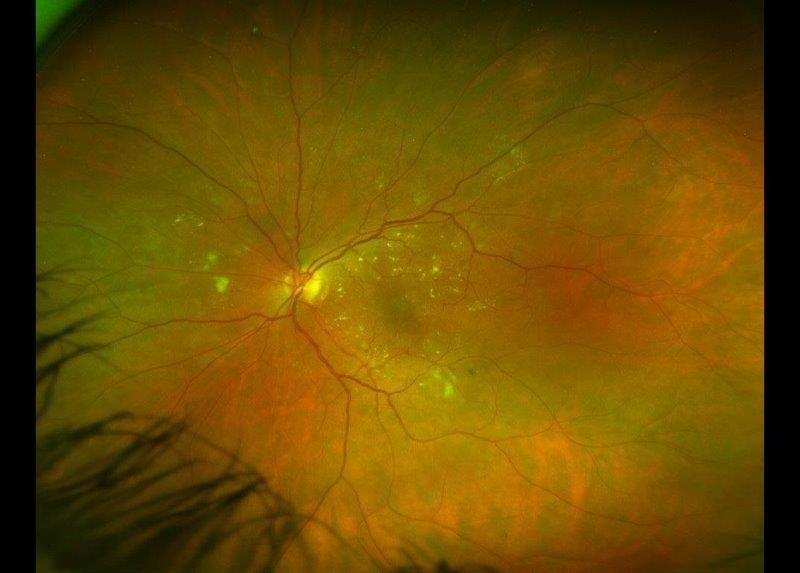
The macula in the right eye showed an indistinct pale area with some fine white mottling within. Optical coherence tomography (OCT) showed outer retinal irregularity with disruption of the ellipsoid zone and focal nodular areas of retinal pigment epithelium (RPE) thickening. There was no subretinal fluid and the OCT appearance was relatively unremarkable given the extent of vision loss (Fig 1). There was a large area of abnormal hyper-autofluorescence within the macula, correlating with the pale lesion seen, as well as a few satellite lesions (Fig 2).
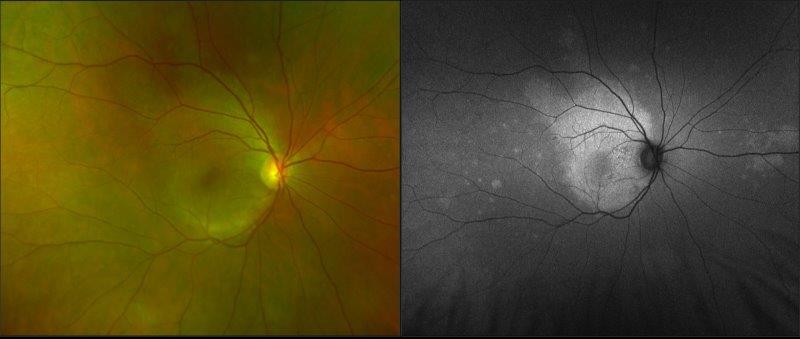
Fig 2. Colour and AF images of right macular showing the lesions are more readily demonstrated on AF
The clinical appearance was very suggestive of acute syphilitic placoid chorioretinopathy (ASPCC) and serological tests soon confirmed he had syphilis. Lumbar puncture also showed positive treponemal tests and he subsequently received two weeks of intravenous penicillin with oral prednisone cover. At the last follow up, vision had improved to 6/12.
Discussion
Syphilis infections are again increasing in New Zealand, with more than 700 cases reported through the mandatory surveillance system in the past year. In the last three months alone, we saw five new cases of ocular syphilis through the uveitis clinics in Auckland. Syphilis can cause any type of uveitis and is termed ‘the great masquerader’ for this reason. ASPPC is one of the rarer types where the clinical appearance strongly suggests the disease.
ASPCC can be unilateral or bilateral and patients present with acute or subacute reduction in central vision. There can be a range of presenting visions, from 6/6 to counting fingers. Other uveitis features can also be present in varying degrees. More than 80% have some anterior chamber or vitreous cells, while other signs, such as retinal vasculitis or retinitis, are occasionally present. It can be a subtle diagnosis to make clinically and in these cases OCT is a valuable tool. The inner retina is unaffected but irregularity of the outer retina and RPE is a universal feature, with focal nodular hyperreflective spots under the retina. The features can appear mild in contrast to the decline in vision, such as with this patient, so a high index of suspicion is needed, particularly for cases where the reduction in vision does not match the clinical appearance. Consideration of further imaging such as autofluorescence (AF) or angiography is also useful, or refer for a uveitis review.
It is important for eyecare professionals to be cognisant of the increasing incidence of syphilis in New Zealand and to exclude it in all cases of uveitis or unexplained acute retinopathy or maculopathy, as the diagnosis has important health implications. Without treatment the consequences of tertiary syphilis can be severe and include dementia. Up to 40% will also have HIV co-infection. Most patients will have a good visual outcome with ASPPC treatment, with one series of 16 patients showing median final vision of 20/25, though there was a wide range from 20/20 to 20/150.

Dr Jo Sims is a consultant ophthalmologist with subspecialist training in medical retina and uveitis. She established the combined uveitis immunology clinic at Greenlane Clinical Centre and a uveitis database, which now has more than 3,000 cases and is used for collaborative research projects. She also consults at Eyes and Eyelids in Auckland and is on the board of Macular Degeneration NZ.