Training tomorrow’s dry eye clinicians
Based on its overwhelming success to date, the School of Optometry and Vision Science (SOVS) has increased the services of its Dry Eye Clinic to two sessions per week.
“Patients have appreciated the comprehensive service and always tell us how grateful they are to finally be receiving treatment,” said Dr Marcy Tong, professional teaching fellow and lead optometrist at the Auckland University clinic.
By using an evidence-based approach, based on TFOS DEWS II recommendations, the clinic stands at the forefront of knowledge on dry eye disease, she said. “We have Part V students that receive comprehensive, hands-on training during the clinic sessions and will be competent when they graduate to diagnose and manage dry eye disease.” Students particularly appreciate being able to use the latest technology and observing the direct benefits to patients, added Dr Tong.
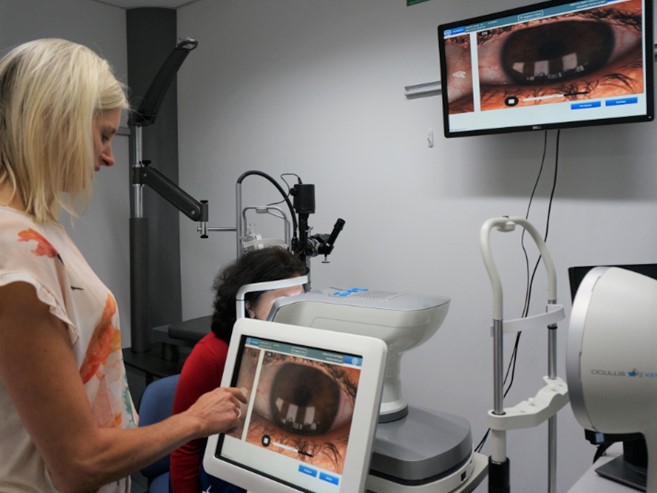
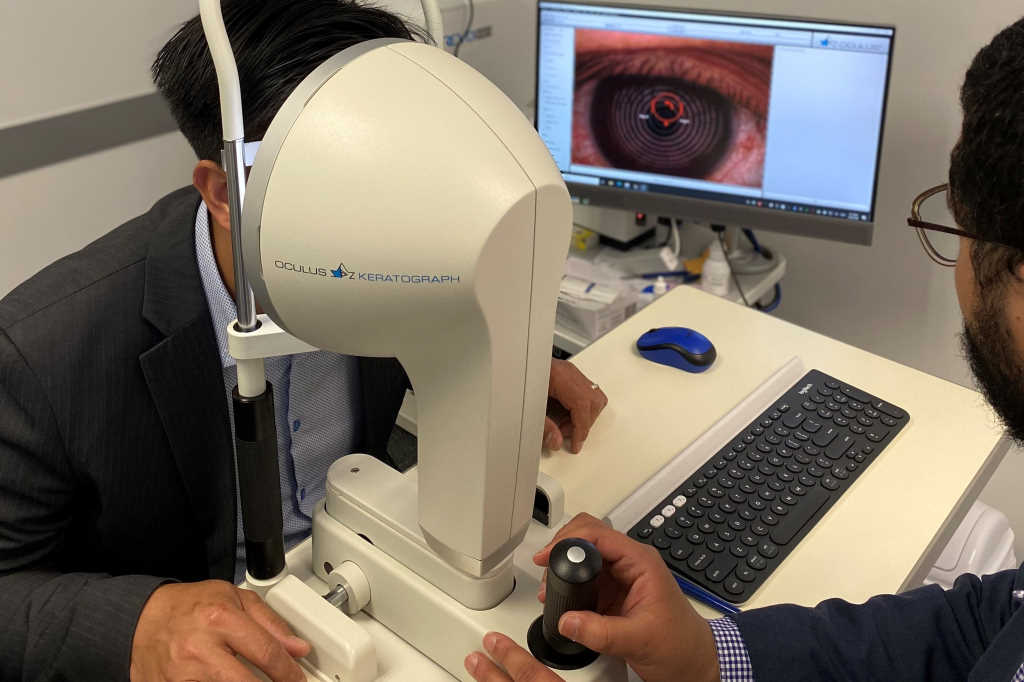
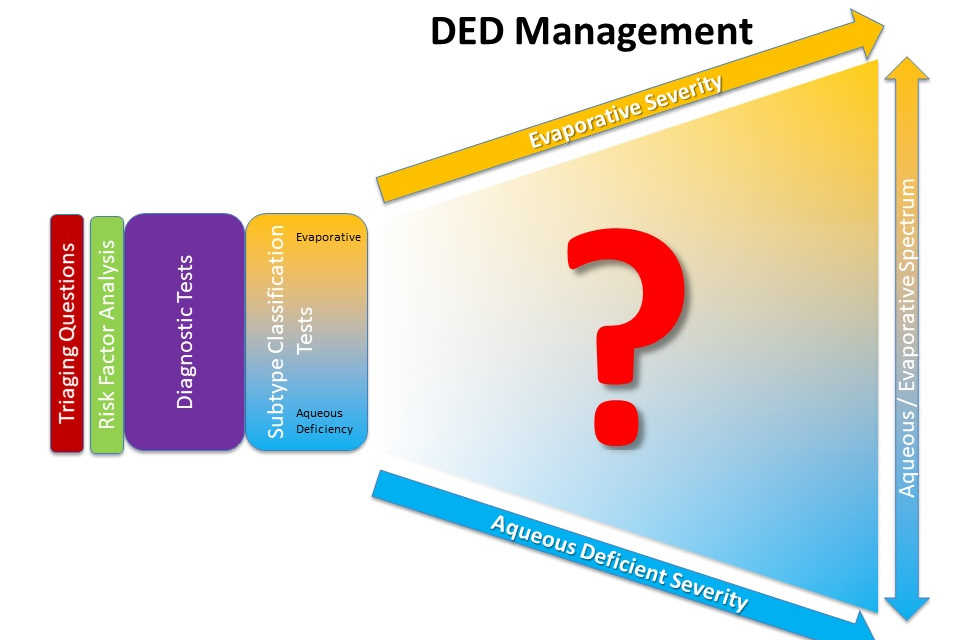
A 90-minute initial appointment at the Dry Eye Clinic includes taking a full history, evaluating signs of dry eye, using both sodium fluorescein and lissamine green, and additional subclassification tests, such as TearLab osmolarity testing and InflammaDry. SOVS is also fortunate to have both a Lipiview II and an Oculus Keratograph 5M to perform the non-invasive tests for dry eye, said Dr Tong. “Using large, wall-mounted screens in addition to our new slit-lamp camera and video, staff and students can educate patients about the specific causes of their dry eye. Patients are offered a full range of treatment options and presented with a step-wise personalised management plan based on their specific history and clinical findings.”
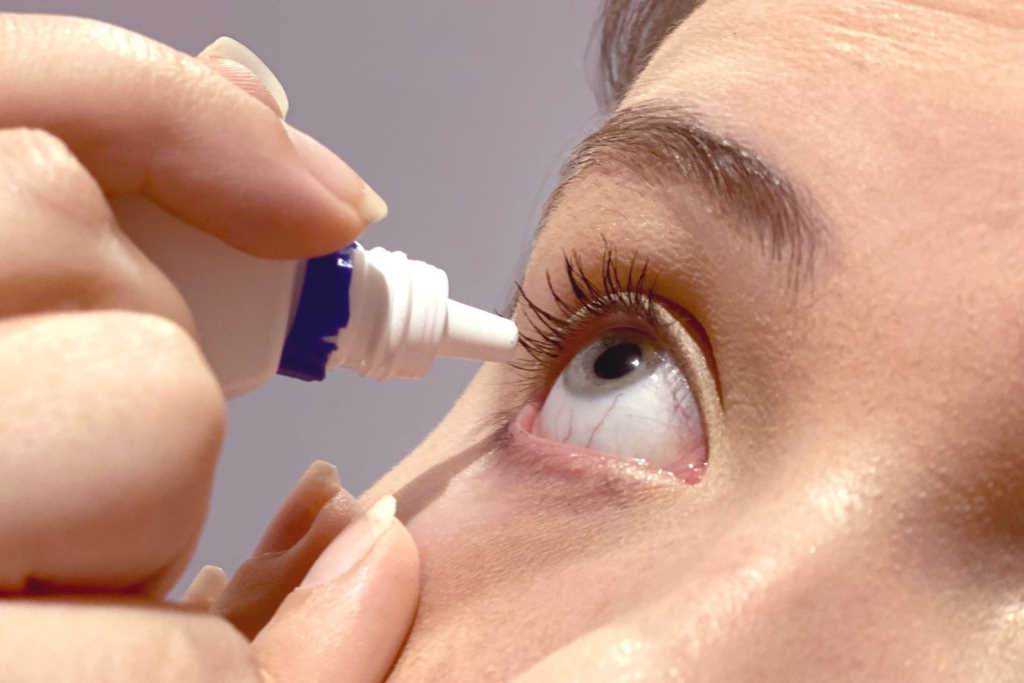
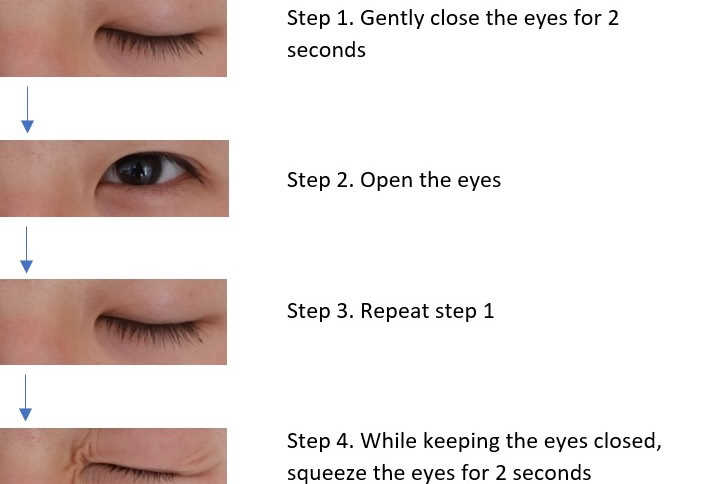
In alignment with TFOS DEWS II recommendations, Dr Tong said she trains students to begin by educating the patient about the chronic nature of dry eye disease and possible environmental modifications. They then demonstrate lid cleansing, lid massage after warm compresses, blinking exercises as well as drop and gel instillation, as required. A direct correlation to the success of treatment has been observed when a patient has a better understanding of their condition and complies with home management, she said.
The patient’s dry eye management plan is then re-evaluated at the next appointment to determine the patient’s progress, so it can be amended according to the patient’s response, taking into account new research, treatments or tips as these emerge, said Dr Tong. “At this stage, the students are able to discuss other available in-office treatment options such as the Blephasteam with gland expression, BlephEx ‘deep’ lid cleansing, IPL (intense pulsed light) or Lipiflow therapy. The long-term, follow-up care is recognised to be critical to successful outcomes and satisfied patients.”
Associate Professor Jennifer Craig, head of the Ocular Surface Laboratory at the University, has been involved since the clinic's inception and has supported its development. She is extremely proud of the clinic’s work, student training and the expansion of its services, so more patients, many of whom have suffered with DED for a long time, can be helped, she said. “It is a fulfilling specialty and a privilege to watch future eyecare professionals being inspired to learn new techniques to better manage their patients of the future, as the demand for dry eye therapy increases.”