Assessing advances in dry eye technology
Research in dry eye disease has gained momentum – in part due to the recent publication of the Tear Film and Ocular Surface Dry Eye Workshop II (TFOS DEWSII) report, a culmination of more than two years of hard work under the auspices of Dr Dan Nelson and New Zealand’s own A/Prof Jennifer Craig – and in part due to the acceleration in technology available in this area. At UNSW in Sydney we have been fortunate to be able to work with two such pieces of technology: the Lipiview interferometer (TearScience Inc, Morrisville, NC, USA) and the Oculus Keratograph 5M (Oculus, Arlington, WA, USA). Prior to using these instruments, we studied their repeatability in order to establish their clinical utility and subsequently conducted a study evaluating the impact of ocular lubricants on the variables measured by these instruments.
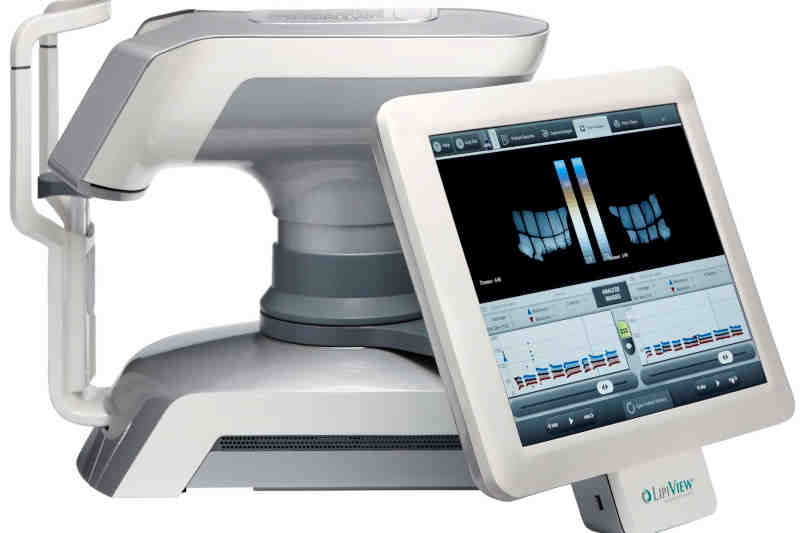
The Lipiview measures lipid layer thickness objectively by transforming the colour interference patterns produced into quantifiable interferometric colour units. The Oculus, among other things, measures non-invasive break-up time (NIBUT), also objectively, by projecting 22 ring mires onto the cornea. The NIBUT is taken as the time between the last blink and the first distortion detected in the grid images by the computer software. We compared these instruments to the Keeler Tearscope-Plus (Keeler, Windsor, UK), a hand-held interferometer used in conjunction with a slit-lamp biomicroscope, that enables both NIBUT and lipid layer thickness to be measured non-invasively, but subjectively. We found the Tearscope to be the most variable of the instruments when it came to measuring NIBUT and assessing lipid layer thickness. Moreover, the Tearscope NIBUT values were significantly higher than those found with the Oculus, and the lipid layer thicknesses were high compared to the Lipiview. We also found that the Lipiview lipid layer thickness was positively correlated with comfort, suggesting it may be of value as a biomarker for dry eye disease.
The Lipiview and the Oculus were subsequently used to determine the impact of lubricants on lipid layer thickness and NIBUT. Twenty participants attended three visits, receiving one of three drops at each visit. The drops given were Optive (Allergan, Irvine, CA), Optive Advanced (Allergan, Irvine, CA) or saline and they were monitored before drop instillation and 5, 15 and 60 minutes after drop instillation. Optive drops are an aqueous-based tear film supplement consisting of carboxymethylcellulose sodium, while Optive Advanced is a lipid-based tear film supplement consisting of the same components as Optive with the addition of polysorbate-80 (0.5%) - designed to deliver castor oil to the tear film.
We found that Optive Advanced significantly increased lipid layer thickness for the first 15 minutes following instillation and that, by the one-hour point, lipid layer thickness had returned to baseline thicknesses. The other two drops did not change lipid layer thickness during the observed period. Despite the improved lipid layer thickness with Optive Advanced, this did not translate to an improvement in NIBUT for any of the drops observed, suggesting that their effect on dry eye may be via another mechanism, such as osmoprotection. Our results suggest that more regular dosing is required to achieve a longer residence of Optive Advanced in the tear film.
With more advances in the technology available to assess dry eye disease, we will be able to better understand the disease and the efficacy of treatments available.
Dr Maria Markoulli is an optometrist, lecturer and researcher with the School of Optometry and Vision Science at the University of New South Wales in Australia. Her research interests include tear film biochemistry and the ocular surface, corneal dystrophies, dry eye disease and contact lens research and development.