Choose your words carefully
In eyecare, some of the most life-changing diagnoses are also the most common. For clinicians, they sit within well‑worn management pathways. For patients, they often mean uncertainty, a loss of independence and perhaps even a life‑changing fear of blindness.
It’s in this place that language can either strengthen a patient’s commitment to treatment or amplify fears that may cause them to withdraw, delay or avoid follow‑up altogether. It’s exactly the space in which healthcare communication consultant and trainer Rachel Callander thrives.
With the goal of ‘humanising healthcare’, she’s passionate about offering clinicians and practice managers simple tools that turn these high‑stakes discussions into opportunities for reassurance, clarity and reduced anxiety.
Lessons from Evie
Callander’s work in health communication was inspired by personal experience when her late daughter, Evie, was born with a rare genetic condition. Over the two-and-a-half years of Evie’s life, Callander gained an insider’s view of the language used across clinics, wards and waiting rooms. She saw how some words added a layer of unnecessary pain, while others offered just enough hope to help patients and their families keep going.
Those experiences set her on a near-decade-long journey exploring both the positive and negative impacts of language used by health professionals. In workshops and keynote addresses across the globe, including in her native New Zealand and her new home, Australia, she has shared her knowledge with staff working in diverse settings, from hospitals to universities to the optical world – most recently at the 2025 RANZCO Annual Scientific Congress in Melbourne.
Diagnosis – the fear factor
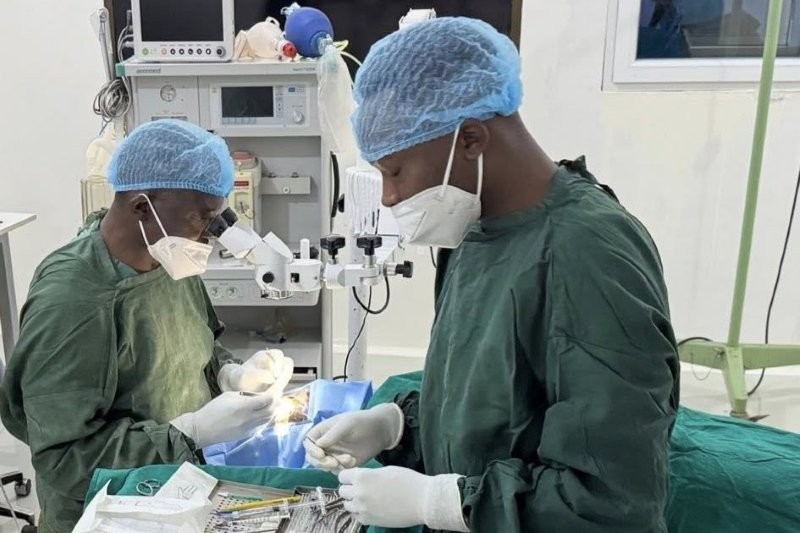
The words used at diagnosis can shape a patient’s perception of their future, but they can also impact how they view you as their clinician. Optometrists often deliver the first shock, perhaps during a routine check when a patient suddenly hears they’re showing signs of glaucoma or retinal disease, with a possibility of permanent vision loss. Ophthalmologists then step in to deliver the procedural reality of scans, medication and surgical options, along with their risks.
“One of the biggest things to realise is how prevalent fear is in many people. That fear can derail the entire conversation because they can shut down,” says Callander. She says a good first step for clinicians is to recognise this fear and how it might impact the message they want to get across. The next is to think about how setting expectations at the start of an appointment can reduce anxiety and signal there’s ample time for both parties to be heard. She suggests opening with something like: ‘We’ve got half an hour together today. I have some important things to talk about with you, but I also want to make sure we cover any concerns you have.’
After delivering the diagnosis and speaking through initial patient questions, Callander recommends building a short follow-up appointment into the care pathway to deal with possible overload. “You can say, ‘I’ve given you a lot of information and you are likely to have a lot of emotions. But I’m with you throughout this and I’m going to do what I can to help ensure that this new life is as smooth as possible. You’re sure to have more questions, so when you go home, write them down and we can speak in a week or so and go through your concerns together.’”
Another aspect she says is often overlooked, one that presents as “a massive opportunity”, is considering the entire patient journey, from the phone call or email to arrival and departure. Reception staff can do some of the ‘heavy lifting’ by creating emotional calmness before patients even reach the consulting room. Simple prompts, such as a paper or digital questionnaire, can invite them to think of questions they want to ask. Callander suggests framing it as ‘Help us to help you by understanding what your concerns are and what you’d like to get out of our time together’.
Openers and closers that count
While fear can affect a consultation, confusion can be just as overwhelming. In her own experience as a parent, Callander remembers not understanding the words clinicians were using. “I didn’t even know how to spell them,” she says. “You’re so confused and then you get angry, because feeling confused makes you feel stupid. And feeling stupid makes you feel even angrier.”
This confusion-driven rollercoaster of emotions has many downsides. Patients may come back with the same questions over and over again and waste time, or they might not even understand enough to follow their prescriptions properly. “Unfortunately, when they come back, they’re not likely to be kind and calm if things go wrong, like if their appointment runs late. They’ll be the quickest ones to get vocal and this has follow-on effects on your staff. The whole place can become emotional very quickly!” Callander says.
That’s where she points to the value of strong consultation openers and closers. “It might be a simple, ‘Do you know why you’re here?’, as some patients get referred and aren’t sure why. Others may not even know what an ophthalmologist is,” she says.
“Other good openers are ‘What is your understanding of your condition?’, ‘How is it impacting your life?’ and ‘What are you hoping to get out of your time here today?’. These can reveal gaps and give you a starting point to match your patient’s reality.”
At the other end of the consult, Callander suggests protecting a small window of time. “If your consultation is 30 minutes, spend the first 20 covering what you need to say. This gives you leeway at the end to ask some really powerful closing questions,” she says.
While Callander has many such questions up her sleeve, she’s found one of the most important is ‘Is there anything you’ve heard me say today that you are going to go home and Google?’
“From that answer, you can tell if they’ve really understood what you’ve said. And as we now live with Google, AI, misinformation and self-diagnosis, this question also gives you the opportunity to direct them to reputable websites that provide clear and accurate information.”
Shifting the mindset
While limitations associated with diagnosis – such as driving restrictions, work changes or loss of visual function – are often major sources of patient stress and fear, they are not the whole story.
“I advocate for a focus on what is still achievable within the diagnosis – looking at the quality of life that is still possible, rather than only what needs to be fixed,” she says. “Some patients can get into their own heads and start losing hope and ability in more areas than just their eye.”
Callander recognises this is a big shift for clinicians trained to diagnose and treat the problem at hand, but is quick to point out that accuracy still matters. For instance, the term ‘retinal detachment’ is medically necessary, but you can pair the stark facts with context and a plan. An example might be: ‘You have a retinal detachment. That means the light-sensitive layer at the back of your eye has started to lift. It sounds scary, but we’ve caught it quickly and can act on it, which increases the chances of a good outcome.’
For clinicians who embrace this broader view, the benefits are wideranging. “They become the professionals at the top of their game; they’re sought after, they’re the ones patients trust most,” she says.
In the end, Callander says, it boils down to one deceptively simple question: how does a patient feel when they leave your clinic? “Do they feel seen, heard and valued? That’s what people are looking for, not shiny gadgets or fancy waiting rooms,” she says.

Renee Lunder is an Australian freelance journalist, proud specs wearer and regular contributor to NZ Optics.