NOSA 2022: in the mind’s eye
After a three-year gap, the Neuro-Ophthalmology Society of Australia (NOSA) held its 36th clinical and scientific meeting in June 2022 in Canberra.
Speakers from neuro-ophthalmology, neurology and even optometry backgrounds presented their research to in-person attendees and virtually. The conference covered topics ranging from emerging serological biomarkers for various conditions including optic neuritis; predictive value of clinical tests for neuro-ophthalmic conditions such as multiple sclerosis (MS), optic neuritis and lesions causing chiasmal compression; and even novel treatment interventions and paradigm shifts for conditions such as idiopathic intracranial hypertension.
A unique feature of the conference was the input of neuropathologist and head of anatomical pathology at Melbourne’s Alfred Health, Professor Catriona McLean, and Canberra Hospital neuroradiologist Dr Shivendra Lalloo, who shared clinical pearls about the interpretation of pathology and neuroimaging, respectively, during the different presentations.
New frontiers
With patents used in the frequency doubling technology and matrix perimeters sold by Zeiss, Professor Ted Maddess’ Australian National University (ANU) team, The Maddess Group, is now working on the world’s first objective visual field test. The objectiveFIELD analyser (OFA) is a multifocal pupillographic perimetry device using stimuli presented ipsilaterally on the right and left of the patient using mirrors while the patient maintains a binocular forward-facing position. Concurrent assessment of both eyes means the test takes less than 85 seconds. If perceived by the patient, the independently presented stimuli will lead to a direct and consensual pupil constriction, which is measured in response to each stimulus, with stimuli presented in many parts of the visual field. This has the advantages of no limitations related to dexterity of the patient and assessment of afferent and efferent visual pathways. Of course, its use is limited if the patient has iris trauma or a fixed pupil.
In earlier iterations, the patient’s fixation was monitored manually, but there is now a gaze tracker. Fixation loss is not reported as a value but rather a regression model of data analysis is used: an excess of data is obtained so up to 15% of it can be discounted if it is associated with loss of fixation or blinks.
As Prof Maddess and Maddess Group member Dr Corrinne Carle said, several studies seem to support the utility of OFA in diagnosis and monitoring of disease progression in MS, even when the subject had not experienced optic neuritis. This has potential, with optic neuritis accounting for only about 20% of first presentations of MS.
Another potential application of OFA was in patients with concussion, since thicker retinal regions were significantly associated with abnormally short delays on OFA.
Nervous disposition
Another new frontier discussed was in the area of neurotrophic keratopathy (NK). Patients with this condition have a degeneration of branch V1 of the trigeminal nerve. This disrupts the afferent pathway of the corneal reflexes (blink, lacrimation) and leads to hypoesthesia (or even anaesthesia), leading to corneal epitheliopathy, impaired vision and even ulceration, perforation, or corneal melt.
Sydney University’s Dr Brendon Lee discussed corneal neurotisation, a new technique involving the transfer of healthy nerves to restore corneal sensation reflexes in patients with NK to enable epithelial healing. This can be from a donor (supratrochlear allograft) or even an autograft from the patient’s sural nerve. This is the first NK treatment with the potential to rehabilitate corneal nerves rather than manage symptoms alone. His team’s work showed improvements with patients’ Schirmer test results and corneal sensation (as measured by Cochet-Bonnet aesthesiometer).

Dr Brendon Lee
Novel applications of existing tools
Dr Anna Britton, from the University of Sydney Save Sight Institute, described how obstructive sleep apnoea (OSA) is a risk factor for vascular disease, explaining studies showing how it alters retinal arterioles and veins. Studies on its effects on microvasculature have yielded conflicting results, however, she said. After investigating retinal microvasculature using OCT angiography, her team’s results showed retinal vessel density is negatively correlated with apnoea-hypopnoea index (events/hours), with untreated patients with more obstructive sleep apnoea having narrower retinal vessel densities. They also found that adequate treatment with continuous positive airway pressure (CPAP) improved capillary plexus vessel density and reversed the narrowing effect. These changes could reflect systemic changes associated with OSA and the systemic vascular changes associated with CPAP treatment. There is also scope for retinal vascular parameters to be a biomarker in the future¹.
I have previously discussed the diagnostic power of ganglion cell analysis (GCA) vs retinal nerve fibre layer (RNFL) OCT measurements for several neurological conditions, including Parkinson’s disease and multiple sclerosis²,³. Dr Jōs Meyer was part of a team that studied the diagnostic power of these tests on recovery from lesions that caused compression of the optic chiasm (pituitary or parasellar tumours). Post chiasmal decompression, RNFL and GCA scans were obtained to see if there was a relationship between either and visual prognosis. They found associations between GCA and recovery and maintenance of long-term (by two years) visual outcomes. Increased thickness of the superior ganglion cell layer was associated with higher odds of long-term visual-field recovery.

Dr Jōs Meyer
Dr Minh Nguyen and her team looked at the predictive power of long-term visual outcomes measured by low-contrast letter acuity (LCLA) and axonal loss (RNFL and multifocal visual-evoked potential) following acute optic neuritis. They found that LCLA at six and 12 months was best predicted by colour vision deficits detected through 38-plate Ishihara asymmetry between the eyes at one month post-acute-presentation of optic neuritis. They also found that LCLA at one month correlated with axonal loss measurements at six and 12 months. The benefit of this is RNFL can give inaccurate information in the first three months due to oedema and conduction block, so there could be utility in performing monocular colour vision testing during this time to help gauge the patient’s long-term visual outcome.
Of course there is a limitation in this pilot study, since the Ishihara test is not great for diagnosing mild deuteranomalies or tritan defects. In the future, larger studies with Hardy-Rand-Rittler pseudoisochromatic plates can be performed.
Another highlight of Dr Nguyen’s presentation was hearing about the @neuroptic Instagram account she co-runs. It’s worth following for useful infographics that make understanding neuro-ophthalmic conditions and clinical tests much easier and more engaging!
Neuro-ophthalmological impacts of Covid
ANU and Canberra Health Services’ Dr Saymaa Selman presented some literature related to neuro-ophthalmic manifestations of Covid and its vaccines. Covid infection can lead to direct neural invasion, endothelial dysfunction, hypercoagulability and even cause a cytokine storm. Subsequently, rare neuro-ophthalmic presentations include associated cranial nerve palsies, optic neuropathies, intracranial hypertension and sequelae of cerebrovascular events. For this reason, Covid can be a neuro-ophthalmic mimic, said Dr Selman, with presentations happening anywhere from preceding respiratory symptoms to developing months after recovery. So it’s good to keep this in mind when encountering patients with acute neuro-ophthalmic presentations, such as pupil changes, vision loss, papilloedema, nystagymus and even diplopia, particularly in patients with neurological presentations who experienced long-duration Covid, had few respiratory symptoms and who lack typical vascular risk factors.
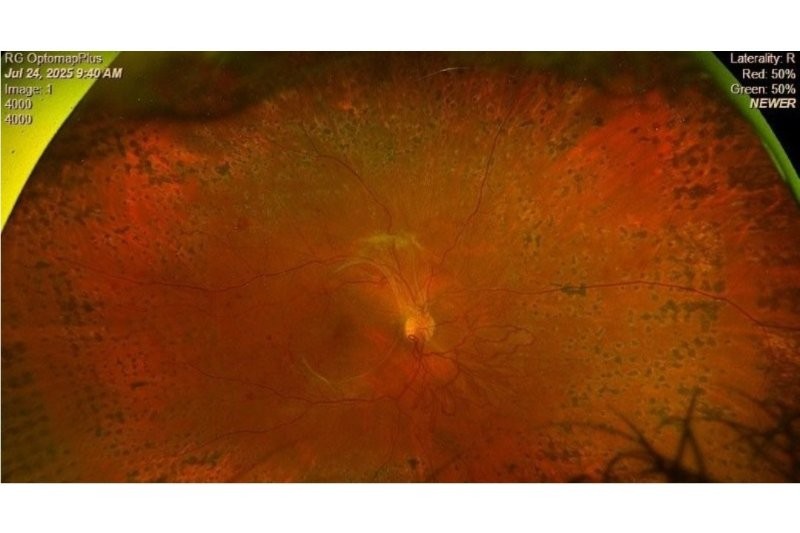
Dr Selman also reviewed ocular manifestations of Covid, which are primarily fundus nodules in the macula (most often bilateral). However, it’s important to note the association is not proven, so it is difficult to correlate ocular manifestations with MRI/neurological imaging.
References
- www.nzoptics.co.nz/articles/archive/probing-sleep-apnoea-and-glaucoma-link
- www.nzoptics.co.nz/articles/archive/case-study-the-importance-of-spotting-microtremors/
- www.nzoptics.co.nz/articles/archive/trusting-tech-and-your-instincts/


Australia-based optometrist Layal Naji is a lecturer of optometry at the University of Canberra and co-founder of the outreach optometry clinic at the Asylum Seekers Centre in Newtown, Sydney.