Pre and post-op drops got my BAK up
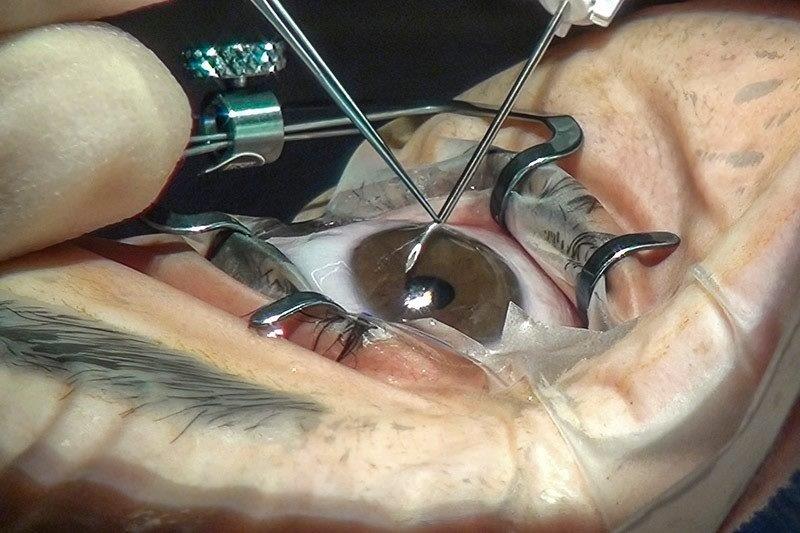
I had cataracts – nothing else. No dry eye, no light sensitivity, no ocular surface discomfort. I had never struggled with irritated lids, gritty eyes or blurred vision beyond what could be attributed to lens opacity. So I underwent same-day immediate sequential bilateral cataract surgery (ISBCS) expecting clearer sight and a straightforward recovery. Instead, I emerged with an ocular surface condition that has reshaped daily life for more than two years.
The trigger, as I now understand it, was exposure to benzalkonium chloride (BAK), a preservative used widely in ophthalmic medications in New Zealand. While reactions such as mine are uncommon, BAK-associated ocular surface toxicity and dry eye disease (DED) are well recognised in the literature, particularly among susceptible individuals.
Immediately prior to entering theatre, four BAK-preserved drops were administered to each eye and the surgery proceeded uneventfully until near the end of the second eye. As the anaesthetic wore off in my first eye, a mild stinging sensation developed. Within minutes, the pain became excruciating. It felt as though acid had been poured onto the surface of my eye: intense burning, rawness and a searing intolerance to light, even through closed lids and protective covers. My eyes streamed with reflex watering; additional anaesthetic provided immediate but short-lived relief. Soon after, the second eye developed identical symptoms. I was given BAK-preserved drops to use at home.
Although the most extreme pain settled after around 48 hours, rawness of the ocular surface, aching, heaviness and marked light sensitivity persisted (fluctuating from initially debilitating to now mild). Incidentally, my surgeon told me that pain medication wasn’t useful for eye pain. So, for many weeks, I did not take pain relief. I eventually used two Panadol every four hours, which helped greatly.
Postoperatively, I was also prescribed prednisolone acetate for two weeks initially and then extended another six weeks due to ongoing inner eye inflammation. Each application triggered two to three hours of greater surface inflammation, aching and photophobia before lessening in time for the next dose. I was reassured this was normal and, compared with the initial acid-like pain, the symptoms felt survivable and I was grateful the worst had passed.
However, vision in one eye became markedly blurred during the early postoperative period (prompting an after-hours ED visit and referral back to the ophthalmologist) and, over the first three to four months, I had recurrent corneal epithelial abrasions and experienced a secondary infection requiring antibiotic treatment.
Identifying the suspects
By experimenting cautiously with my drops, I was able to determine the drops themselves were aggravating my symptoms. At week two, my ophthalmologist advised stopping the non-steroidal drop because of its preservative, described to me as “nasty”. On checking, I discovered that prednisolone acetate drops contained the same preservative – BAK. So I left a message with my clinic requesting a preservative-free (PF) steroid, which went unanswered for six weeks.
At my eight-week appointment the steroid drop was stopped immediately and I was discharged with a report diagnosing “blepharitis posterior and anterior components”. The report also stated I had this prior to surgery. However, neither my referring clinician nor my surgeon ever spoke of blepharitis prior to surgery. Nor did I have any symptoms of blepharitis before or after surgery. So that diagnosis never sat comfortably with me. My eyelids have never been itchy, crusted, scaly or greasy and I have never experienced a foreign-body sensation. My postoperative problem is confined to the ocular surface: rawness, aching, heaviness and light intolerance. My understanding is my symptoms are consistent with nerve-mediated ocular surface injury after cataract surgery related to BAK-preserved drops, with prolonged recovery.
After stopping the steroid drop, I had three days where my eyes seemed much more settled but the rawness on their surfaces remained. My symptoms then worsened, consistent with rebound inflammation. An optometrist, consulted initially for reading glasses, noted ongoing intraocular inflammation and no signs of blepharitis. He urgently referred me back to ophthalmology, recommending a tapered course of PF steroid. This proved pivotal. A three-week tapered course of PF dexamethasone gel resolved the inner eye inflammation completely, without any adverse reaction.
At about the six-month mark, my concern at the slow healing and several separate incidences of abrasions and one infection requiring antibiotics, led me to see a corneal specialist, who diagnosed: “Disturbance of tear film and corneal epithelium by topical anaesthetics, surgery and post-op drops”.
A preservative-free future
My eye surfaces have remained 'edgy' and vulnerable as the nerves have continued to regenerate gradually over the last 24 months. I still have variable but persistent ocular surface sensitivity and rawness. Triggers such as wind, heating, smoke, eye makeup and light – none of which troubled me previously – all worsen symptoms.
After trialling numerous products, carbomer-based drops provided the most sustained relief, supplemented by PF lubricating gels during flares and at night. More specifically, I now rely on six to 20 drops a day alternating between Evolve Carbomer 980 and Hylo-Forte, and Poly Visc gel, when needed for the worst days and nights. During difficult episodes, I awake multiple times to soothe my eyes. Although my visual acuity is good, discomfort still affects my ability to work for sustained periods as an artist, tutor, author and video presenter. To counter this, I’ve bought specially sealed Bolle safety goggles, which have become essential during winter months and when the home heating is on.
During this time period, a later secondary posterior capsulotomy, performed by a different ophthalmologist using only PF medications, caused no reaction or difficulty of any kind.
From my perspective as a patient, several lessons stand out:
• Susceptibility to BAK may not be apparent until exposure occurs, yet its ocular surface neuro-toxicity is well established. Screening or patch-testing for hypersensitivity could help identify at-risk patients.
• ISBCS relies on treating each eye as though it belongs to a different patient. Administering BAK-preserved drops to both eyes simultaneously removes the opportunity to identify intolerance before bilateral exposure.
• Patients should be informed clearly about the medications they receive and offered a genuine choice between preserved and PF options, alongside an explanation of potential risks.
• Effective pain relief may spare others a long and difficult road.
• The long-term cost – medical, personal and economic – of BAK-related injury far outweighs short-term savings.
I am sharing my experience not to apportion blame, but to highlight what I believe is a potentially avoidable cause of long-term, life-altering pain for some patients. My hope is that increased clinician awareness will prompt discussion, reflection and innovation, particularly around reducing or eliminating BAK exposure where safer alternatives exist. Simple changes may spare others a long and difficult road.
The views expressed by Chalkeyes are theirs alone and not necessarily the views of the NZ Optics team or the publisher, Old Butcher Holdings Ltd. If you wish to comment on Chalkeyes’ views, please email a brief letter to the editor editor@nzoptics.co.nz for consideration. Letters may be edited for space, style, grammar and clarity.