The CLC lab where bespoke lenses are born
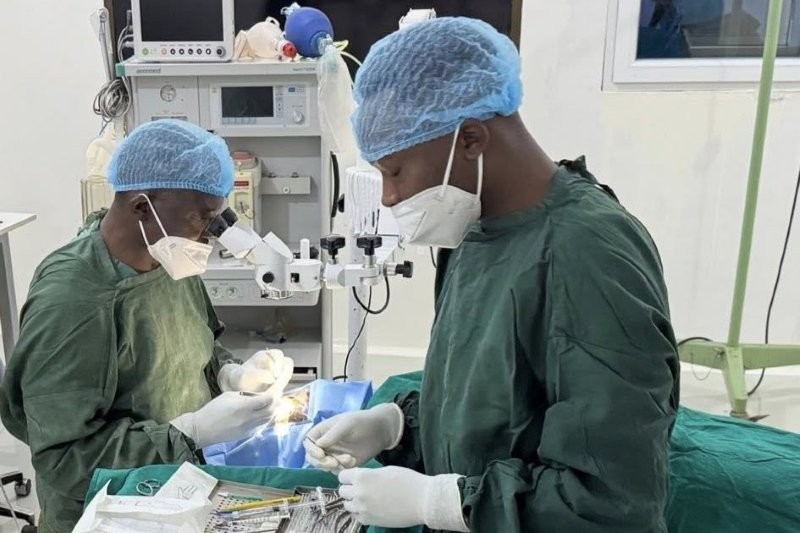
Tucked in behind a modern façade in Wigram, Christchurch, Corneal Lens Corporation’s (CLC) laboratory is manufacturing some of the most complex contact lenses used in New Zealand eyecare. Susie Hill had the good fortune to listen to two talks about the lab’s processes by optometrist and technical consultant Andrew Kim and visited the lab to witness the magic.
When you step out of the taxi, the low-lying lab looks like nothing in particular and is still rather ordinary when you enter the building. Upstairs, phones ring and emails arrive from optometrists around the country. Downstairs, in a tightly temperature- and humidity-controlled lab, diamond-tipped lathes spin at up to 10,000 revolutions per minute, carving tiny ‘hockey puck’ blanks into medical devices that can restore sight where glasses and standard lenses fall short.
CLC manufactures about 50,000 rigid lenses and 4,000 soft lenses each year, along with distributing eyecare solutions. Every one of those lenses is fully custom made, not just for a patient, but for an individual eye. There is nothing off the shelf. The lab is where prescription, topography and design theory collide with engineering realities, quality systems and a surprising amount of human touch.
The upstairs-downstairs partnership

CLC lab technical consultants Alan Benjamin and Andrew Kim
On the office level, CLC’s technical consultants, including Andrew Kim, act as a bridge between practitioners and the lab. Many of the cases that land on his desk are at the far end of complexity. An optometrist may face a keratoconic cornea that does not match their usual designs, an aphakic baby who needs a very high plus soft lens, or a long-term rigid wearer whose irregular cornea is now challenging their current fit. Sometimes a lens that should work perfectly on paper simply does not perform on the eye. Andrew tells us that is when collaboration becomes essential. Practitioners send through refraction, topography maps, previous parameters, slit-lamp findings and patient goals. He helps them choose a design, refine starting parameters and understand trade-offs between vision, comfort and corneal health.
Even at the ordering stage, precision matters. “A comment such as ‘increase lift one step’ can mean very different things depending on the design. Is that one base curve step? A peripheral lift adjustment? An edge change only? Before a lathe ever starts spinning, the technical team often checks previous orders, compares design logic and, if needed, picks up the phone. A significant portion of quality control happens before a blank is ever touched,” Andrew explains.
Why a specialty lab still matters
The need for this level of customisation is driven by real clinical gaps, says Andrew. “For patients with extreme ametropia or prescriptions outside stock ranges, custom lenses may be the only option. For irregular corneas, such as in keratoconus, pellucid marginal degeneration or post-graft eyes, rigid lenses often provide the only functional acuity.”
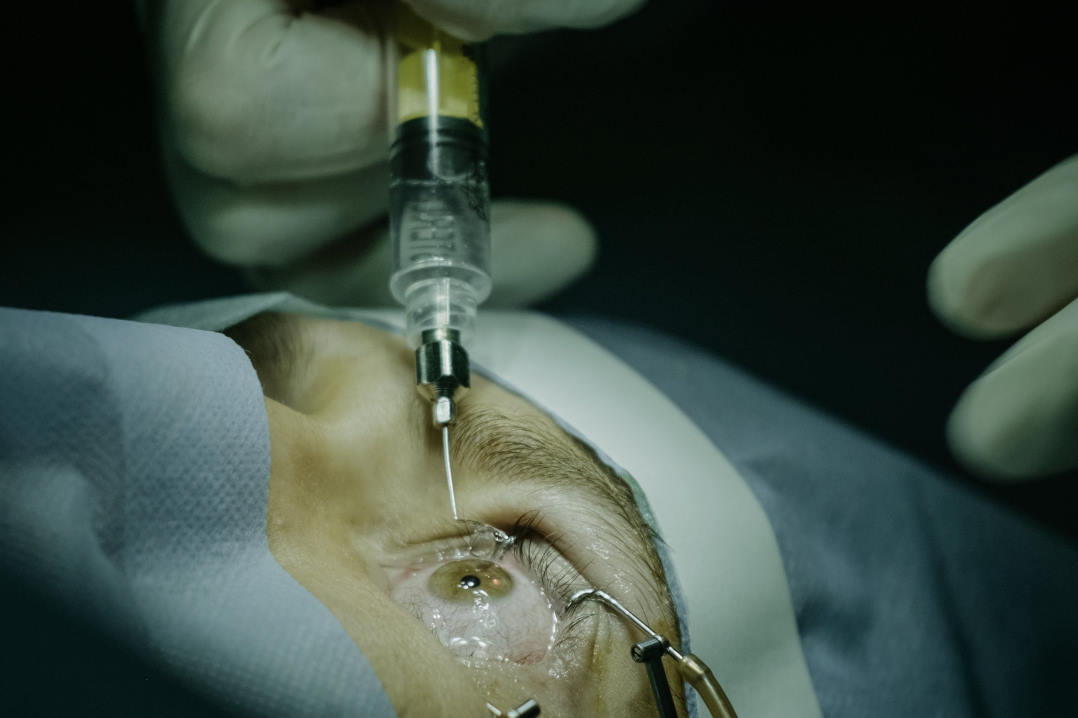
Rigid lenses work because they create a new optical surface. The rigid shell, the tear layer beneath it and the cornea function together as a smooth refractive system, masking underlying irregularity. There are also ocular-surface indications. Large scleral lenses vault the entire cornea and land on the sclera, trapping a reservoir of fluid against the eye and protecting the corneas of patients with severe dry eye.
Andrew’s talks describe how myopia control through orthokeratology continues to grow and that cosmetic and prosthetic lenses remain an important part of CLC’s work. Matching iris colour, pupil size and pattern can restore both appearance and confidence. All of this relies on the lab’s ability to manufacture precisely what has been designed.
Measuring the eye in three dimensions
Modern topography underpins much of the design process. Corneal elevation maps guide base curve selection and peripheral design. Newer imaging systems capture scleral shape as well, revealing that eyes are rarely perfectly symmetrical. This information allows lenses to better reflect the real anatomy of the eye rather than relying solely on standard curve systems. Particularly in scleral and irregular cornea work, this level of detail directly influences comfort and stability. The lab must then translate that digital data into physical form with remarkable precision.
Inside the lab: blanks, lathes and diamonds

Nicola May
Lab supervisor Nicola May, who’s been with the lab for 31 years, leads me downstairs into the lab. Along one wall sit trays of colourful blanks, each resembling a small opaque button. It is hard to believe that these unremarkable discs will become life-changing devices. Even soft lenses begin life as hard blanks. It’s difficult to resist touching them all.
Nicola tells me the first step in the lens-creation story is blocking. She attaches a blank to a special tool so it sits perfectly centred on the lathe spindle. If it is not centred, the cut will be inaccurate. Depending on the lens type, this may involve double-sided tape or specialised wax. The blank must remain completely stable at very high rotational speeds.
She explains that they cut the back surface first. The lathe probes the blank to measure thickness, then rough diamond tools remove the bulk of material. These diamonds create the basic concave shape of the back surface. Finer finishing diamonds then skim away tiny amounts of material to refine the optical surface. It’s mesmerising to watch.
Vacuum systems remove debris while compressed air cools both the material and the diamond tip. Heat control is critical, particularly with softer or high-Dk materials (those with high oxygen permeability), Nicola says. Modern lathes can oscillate tools to create toric or asymmetric surfaces. The more complex the design, the slower the spindle must run and the longer the cycle time.
Once the back surface is cut, it receives a very brief polish – experience has shown that minimal polishing preserves optical precision. The aim now is to cut accurately and polish only enough to remove fine machining marks. A team of people works at lens edging and polishing stations, with one stalwart, Lynn, working at CLC for over 40 years! After polishing, the back surface is inspected and measured by hand. Base curve and surface quality must fall within strict tolerances. If not, the process starts again.
Re-blocking and cutting the front

A diamond-tip cutting a lens on the end of the lathe's spindle. Credit: CLC
Once the back surface is complete, the lens is re-blocked. A second tool is bonded to the freshly cut back surface, chosen to match it as closely as possible. The original tool is removed, exposing the front surface. The lens returns to the lathe. The machine again probes thickness, aligns itself using a small drill mark left from the first pass and begins cutting the front surface. Rough diamonds shape the optic zone and establish the correct power. A diameter cut sets the lens size. Finishing tools refine the final surface.
Depending on the design, the edge may be shaped directly on the lathe or refined later by hand. Some lenses require manual edging to soften a slightly square finish left by machining. I then watch as laser engraving adds identifying details to the surface. Each lens leaves the lab as a fully traceable medical device, its laser-etched identifier linked to its complete manufacturing record. Both surfaces are then measured for power, centre thickness, diameter and surface integrity. Only when everything falls within tolerance does the lens move forward.
Soft lenses: hydration and tinting
For soft lenses, the next stage is hydration. After cutting and edging, the lens is placed in solution and allowed to absorb water, often overnight. Each material has its own swelling factor, so once fully hydrated, the lens must be re-measured. Power and diameter can shift slightly as the lens reaches equilibrium. Tinted and prosthetic lenses are coloured at this stage. In a little room of their own, technicians work from reference photos and colour swatches, layering dyes to match iris patterns and tones. Achieving a natural appearance requires patience and skill.
Surface treatments and packaging
Rigid lenses typically undergo plasma treatment, which cleans and activates the surface, improving wettability. Some designs receive additional surface coatings that require curing time before dispensing. Final cleaning and inspection take place in a clean room under positive pressure. Soft lenses are sealed in blister packs and sterilised in autoclaves.
Materials matter
Andrew says material choice influences both performance and manufacturing. Lower water content soft materials tend to be stronger and more durable, making them useful for prosthetic work. Higher water content materials provide greater oxygen transmission and flexibility but are generally less robust.
In rigid materials, lower Dk options are harder and more resistant to scratching. Higher Dk materials are softer and more easily marked. Scleral lenses add complexity because of their size and depth, requiring careful control during cutting and finishing.“Even small changes in blocking compounds, waxes or dye formulations can affect outcomes. Manufacturing is not only about precision machinery but about understanding how every material behaves throughout the process,” Andrew says.
Quality systems and remakes
CLC operates under ISO 13485 medical standards. Any deviation triggers investigation and corrective action. Andrew notes that most remakes arise from human factors during polishing or edging rather than machine error. A small scratch or slight over-edging can mean starting again. Yet the remake rate for rigid lenses remains around 4%, reflecting careful oversight.

A quiet engine of eyecare
Andrew says he believes the best outcomes are achieved when practitioners understand how manufacturing works, communicate clearly about their goals and constraints and are willing to problem-solve together with the lab. “For patients with irregular corneas, severe dry eye, high prescriptions or eyes altered by trauma or surgery, that collaboration can mean the difference between ongoing visual compromise and clarity.”
At the lab’s heart, I saw a team of fun-loving dedicated people, many of whom have made this intricate work their lifelong career and who speak with so much affection for the lab and its late founder and director, Graeme Curtis. Nicola says the relief when the Curtis family decided to stay in business after his passing was immense.
Watching a plain little puck transformed into a bespoke optical device makes one thing clear: specialty contact lens manufacturing is both science and craft. It requires precision equipment and rigorous systems, communication, experience and steady hands. Each lens that leaves CLC carries a chain of decisions, measurements and careful workmanship. In that humble building housing a dedicated team, some of New Zealand’s most complex eyes are being given their best chance to see clearly.